AI-Rx - Your weekly dose of healthcare innovation
Estimated reading time: 4 minutes
TL;DR:
Largest systematic review ever on psychiatric meds and suicide (48 studies, 6M+ patients, 70 medications).
Key finding: diagnosis matters. Second-gen antipsychotics reduce risk in schizophrenia, lithium in bipolar disorder, SSRIs/TCAs in depression. Benzodiazepines associated with HIGHER suicide risk across nearly all diagnoses.
Findings are observational, not causal… but they're comprehensive real-world evidence we've been missing.

Randomized controlled trials on suicide prevention face an impossible problem:
❌ Ethically challenging to conduct
❌ Exclude people at elevated suicide risk
❌ Short duration (weeks to months)
❌ Don't reflect real-world clinical populations
The solution?
Synthesize 30+ years of observational evidence from actual clinical practice.
The result:
The largest systematic review and meta-analysis on psychotropic medications and suicide outcomes ever published.
The Study
Published: The Lancet eClinicalMedicine (March 2026)
Scope: 48 studies from 13 countries
Patients: 6,489,573 people (mean age 41.6 years)
Medications: 70 individual medications across 5 classes
Diagnoses: Schizophrenia-spectrum disorders, bipolar disorder, depression, personality disorders
Study designs:
Between-individual (prescribed vs not prescribed)
Within-individual (on medication vs off medication periods in same person)
Here’s what they found
Initial findings were messy and hard to interpret.
But stratifying by diagnosis revealed clear patterns.
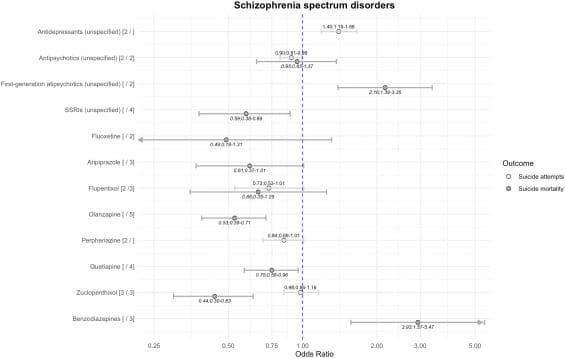
Schizophrenia-Spectrum Disorders
Second-generation antipsychotics associated with LOWER suicide risk:
Clozapine: 60% reduction (OR = 0.40)
Olanzapine: 47% reduction (OR = 0.53)
Quetiapine: 25% reduction (OR = 0.75)
Risperidone: 39% reduction for suicide attempts (OR = 0.61)
Zuclopenthixol: 56% reduction (OR = 0.44)
First-generation antipsychotics: Associated with ELEVATED risk
Benzodiazepines: Associated with HIGHER risk
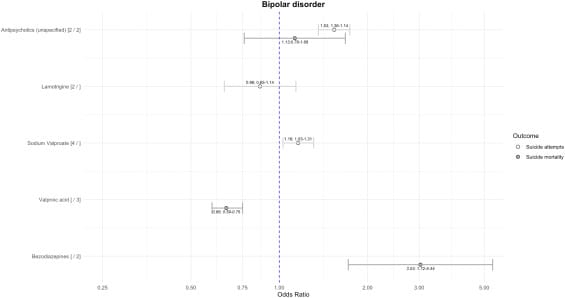
Bipolar Disorder
Mood stabilizers associated with LOWER suicide risk:
Lithium: 62% reduction for suicide mortality (OR = 0.38) 40% reduction for suicide attempts (OR = 0.60)
Valproic acid: 34% reduction for suicide mortality (OR = 0.66)
Benzodiazepines: Associated with ELEVATED risk of suicide mortality
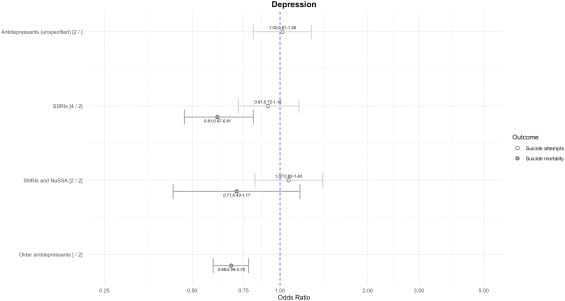
Depression
Antidepressants associated with LOWER suicide mortality:
SSRIs: 39% reduction (OR = 0.61)
Tricyclic antidepressants: 32% reduction (OR = 0.68)
For suicide attempts: No strong evidence in either direction
The Benzodiazepine Problem
Across nearly all diagnostic groups, benzodiazepines were associated with HIGHER suicide risk.
In personality disorders:
Benzodiazepines and suicide mortality: OR = 4.29 (329% INCREASE)
Yet benzodiazepines remain widely prescribed for:
Anxiety
Insomnia
As adjuncts to other treatments
Often chronically

What This Means Clinically
Key Takeaway #1: Diagnosis matters
Medication effects differed substantially across psychiatric disorders. Suicide prevention isn't diagnosis-agnostic.
Key Takeaway #2: Appropriate medication may reduce risk
For specific diagnoses, certain medications showed protective associations:
Second-gen antipsychotics in schizophrenia
Lithium in bipolar disorder
SSRIs/TCAs in depression
Key Takeaway #3: Benzodiazepines need ongoing review
Individuals prescribed benzodiazepines require:
Periodic medication reviews
Monitoring for chronicity
Consideration of whether continued use is justified
The Critical Caveat
These findings are NOT causal.
They're observational associations.
They need triangulation through:
Target trial emulation studies
Mechanistic preclinical studies
Careful clinical interpretation
Confounding by indication is real:
People prescribed first-generation antipsychotics often have more severe illness or haven't responded to other treatments. They're already at higher risk… which may explain associations with poorer outcomes.
What This Doesn't Mean
❌ Medication alone prevents suicide
❌ Everyone with depression should be on SSRIs
❌ Never prescribe benzodiazepines
❌ These medications guarantee protection
Suicide attempts and deaths are relatively rare outcomes—even among people with diagnosed psychiatric disorders. Medications won't prevent all events.
What This Does Mean
✓ Suicide prevention strategies should consider appropriately prescribed medication as ONE component
✓ Pharmacological interventions work alongside psychotherapy, safety planning, crisis intervention, and social support
✓ Diagnosis-specific medication strategies may have a role in reducing risk
✓ Benzodiazepine prescribing requires more caution and monitoring
The Bigger Picture
This study synthesized 30+ years of real-world evidence from clinical practice.
It confirms some long-held beliefs (lithium in bipolar disorder) and adds new evidence (second-gen antipsychotics in schizophrenia).
The question isn't "medication vs no medication."
The question is: How do we build comprehensive suicide prevention strategies that integrate appropriate medication for specific diagnoses alongside all other evidence-based interventions?
Does your organization's suicide prevention protocol differentiate medication strategies by psychiatric diagnosis, or are we treating suicide risk as diagnosis-agnostic?
Dr. Bhargav Patel, MD, MBA
Physician-Innovator | AI in Healthcare | Child & Adolescent Psychiatrist
P.S. Want evidence-based psychiatry insights in your feed? Follow me at LinkedIn.
Read the Full Study:
Kozhevnikova et al., "Effect of psychotropic medications on suicide-related outcomes," eClinicalMedicine (2026)
Lead author: Seena Fazel, University of Oxford